Areas of Clinical Expertise
Carotid artery
- What is a carotid stenosis and what are the consequences?
- How does a carotid stenosis form and how is it diagnosed?
- When must a carotid stenosis be treated?
- What are the treatment options?
- What happens after surgery?
- You can make an appointment here
What is a carotid stenosis and what are the consequences?
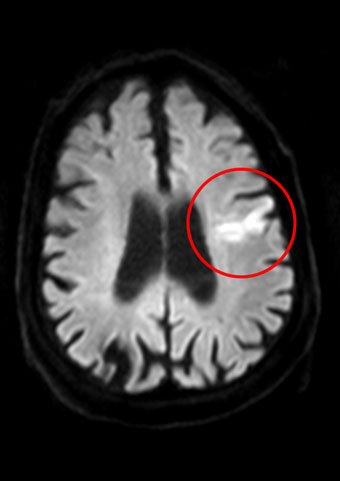
Carotid stenosis is a narrowing (stenosis) of the inner, cerebral carotid artery (Arteria carotis interna). Approximately 15% of people over 70 have a detectable carotid stenosis, which is often discovered as an incidental finding during an ultrasound examination. If there is a significant (<70%) narrowing, there is an increased risk of suffering a stroke. A stroke is the result of a sudden circulatory disorder of the brain.
In the worst case scenario it can lead to permanent damage of the brain tissue, due to lack of oxygen. Approximately 200,000 Germans suffer a stroke each year. Early warning symptoms of stroke include sudden and temporary visual impairment, speech problems and possibly numbness and paralysis of the arms or legs. When these occur, an immediate medical examination is necessary.
How does a carotid stenosis form and how is it diagnosed?
The cause of carotid stenosis is usually arteriosclerosis (hardening of the arteries), when there is a formation of plaque (deposits of blood fats, blood clots and calcium build-up) on the vessel wall with resultant narrowing of the vessel. Risk factors that promote arteriosclerosis include smoking, high blood pressure, blood sugar (diabetes mellitus), high cholesterol and a family history.
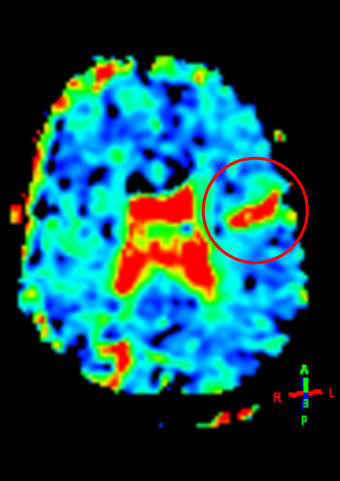
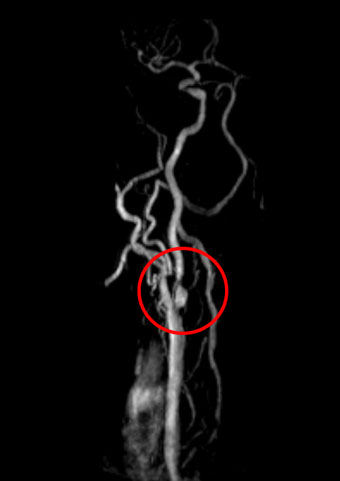
The diagnosis of carotid stenosis is carried out primarily by duplex sonography (ultrasonography), painlessly and without radiation exposure. If findings are inconclusive and for the planning of any treatment, magnetic resonance imaging is performed as a standard procedure (without radiation), with representation of the vessels and the brain. In certain cases (pacemakers, hip / knee replacement) computed tomography is carried out (with X-rays). For detailed information about these and other examination options, see the “Angiology” range of treatments.
When must a carotid stenosis be treated?
For limited narrowing of the carotid artery, regular ultrasound controls are adequate. In severe narrowing of the carotid artery without symptoms, an operation should be considered. For a carotid stenosis with already occurring warning symptoms (blurred vision, slurred speech, paralysis (arms and legs), sudden severe headache, dizziness) or stroke there should be immediate hospitalisation and a timely operation. For an atherosclerotic carotid stenosis, supportive medication (aspirin, statins) should be continued indefinitely. Blood pressure, diabetes and cholesterol should be checked regularly and adjusted to their optimum levels.
What are the treatment options?
- Surgery – carotid thromboendarterectomy
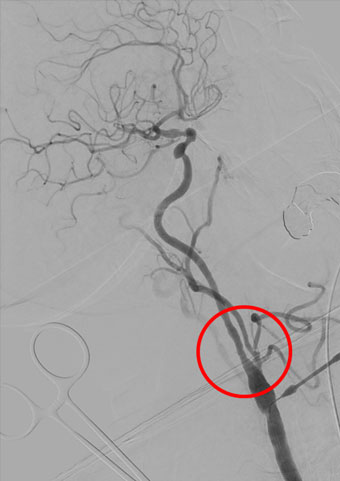
The operation is performed under local anaesthesia or general anaesthesia. During surgery, the carotid artery is exposed via a small incision in the neck and the calcification stripped off. Depending on the findings, reconstruction is carried out with a plastic patch, or the severed vessel sewn directly back on. During the operation, the brain blood flow is monitored continuously to detect blood flow disorders in time. At the end of the operation the results of the intervention are checked by a vascular imaging with contrast medium (angiography).
- Intervention – Carotis-Stent-Implantation
Stent angioplasty (dilation of the vessel and supporting with a lattice framework) of the narrowed carotid artery can be performed both via the groin and also semi-openly through a small incision at the base of the neck (bypassing the aortic arch). This is performed in special cases (patient preference, anatomical reasons) and carried out in the context of the ACST 2 study.
The ACST 2 study (asymptomatic carotid surgery trial) compares the long-term outcome of asymptomatic patients after open surgery and stenting.
Overall, it is a simple procedure that can prevent patients from having a stroke with serious consequences. The hospital stay is usually only a few days.
What happens after surgery?
After the operation and the appropriate recovery period you can exert yourself fully. Four weeks after surgery, an ultrasonic inspection is carried out, gladly in our office. Supportive drug treatment should be continued indefinitely. Blood pressure, diabetes and cholesterol should be checked regularly and adjusted to their optimum levels.
Patient flyer (PDF)
BR-post (YouTube)
You can make an appointment here
 Centre for Vascular Medicine and Polyclinic of the Clinic for Vascular and Endovascular Surgery
Centre for Vascular Medicine and Polyclinic of the Clinic for Vascular and Endovascular Surgery
Ismaninger Str. 22
D-81675 München
Tel.: 089 4140-6666
If you have already had tests, please bring these to your appointment, gladly in CD format if available.

 Notfallkontakt
Notfallkontakt